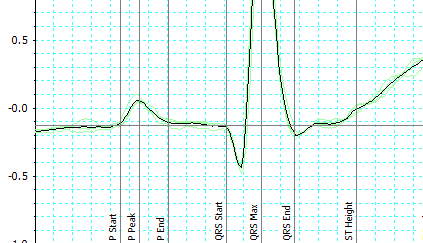
Basal NO production and iNOS expression were also increased by SARS-CoV-2. Genetic deletion of TNFR1 prevented vascular changes triggered by MHV-3, and death. TNF production was increased in plasma and vascular tissue. In the aorta, iNOS and phospho-NF-kB p65 subunit expression was enhanced, along with basal NO production. The contractility of the aorta was normalized by removing the endothelium, inhibiting iNOS, genetically deleting iNOS, or scavenging NO. Resistance mesenteric arteries showed increased contractility. MHV-3 infection reduced aortic and vena cava contractility, arterial blood pressure, and blood flow, resulting in death. Survival curves were estimated using Kaplan–Meier. ELISA was used to assess cytokine production. Nitric oxide (NO) was quantified with the DAF probe. Tail-cuff plethysmography and Doppler were used to assess blood pressure and flow, respectively. Protein expression was determined by immunofluorescence. Isometric tension was used to evaluate vascular function. Wild-type C57BL/6 (WT) and knockout mice for inducible nitric oxide synthase (iNOS −/−) or TNF receptor 1 (TNFR1 −/−) were infected with MHV-3, and K18-hACE2 transgenic mice expressing human ACE2 were infected with SARS-CoV-2.  
Here, we investigated the mechanisms underlying the vascular dysfunction caused by the betacoronaviruses MHV-3 and SARS-CoV-2. Poor disease outcomes and lethality are directly related to endothelial dysfunction in betacoronavirus infections.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
